Allergic Fungal Sinusitis
Allergic Fungal Sinusitis – About
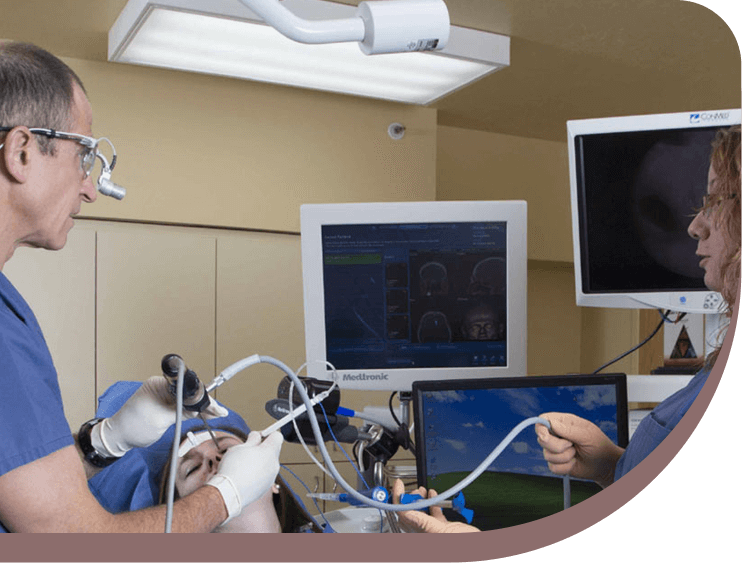
Allergic fungal sinusitis (AFS) is a common type of fungal infection in the sinuses. The infecting fungi are found in the environment and cause an allergic reaction which results in thick fungal debris, sticky mucus and blockage of the infected sinus. Patients with AFS may have allergies, nasal polyps and may have asthma. As a result of the condition, most patients develop chronic sinusitis which may affect their sense of smell. Left untreated, this condition may lead to displacement of the eyeball and vision loss.
Although AFS can occur at any age, allergic fungal sinusitis is more common in adolescents and young adults. After the initial exposure during normal nasal respiration, an inflammatory reaction occurs, causing tissue edema. This results in sinus obstruction and a slowing or stoppage of normal sinus drainage, creating an ideal environment for the fungus to grow.
Patients often have a history of allergies and nasal polyps and many have asthma and chronic sinusitis.
Allergic Fungal Sinusitis – Diagnosis
The presence of allergic mucin (a group of mucoproteins that are found in secretions and tissue) is a reliable diagnosis of fungal sinusitis. A mucus sample is sent to a laboratory where it is examined for signs of fungi. Patients may also be tested for invasive fungal sinusitis, saprophytic fungal growth, mycetoma, aspergilloma, fungus ball of the sinuses and eosinophilic mucin sinusitis to assist in confirming both a positive or negative diagnosis of AFS.
Allergic Fungal Sinusitis – Treatment
Surgical removal of the thick fungal debris and muci in the infected sinuses is the most effective way to treat AFS. Steroids may be given before and after the surgery. Recurrence of AFS is not uncommon and patients may require additional surgeries. Immunotherapy and anti-inflammatory therapy may also be used to eliminate the fungal colonies.
Conditions Treated
Follow us


Your Health Starts Here
"*" indicates required fields
